Skin cancer is the most common form of cancer in the world. Over five million cases of skin cancer are diagnosed in the United States each year; this is more than the number of new cases of prostate, breast, lung, and colon cancer combined. Most skin cancers are associated with ultraviolet (UV) radiation from the sun.
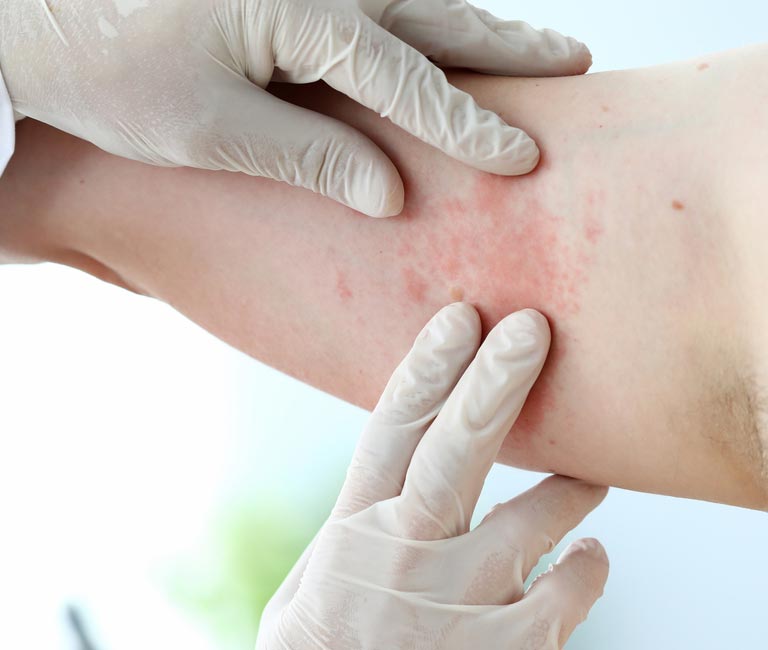
What skin cancer looks like depends on the type of skin cancer. The most common types of skin cancer, squamous cell carcinoma and basal cell carcinoma, may present as pink or red sores that do not heal. They sometimes itch, hurt, or bleed. Melanoma sometimes appears as a mole with several shades of brown, black, pink, purple, or red. The border may be uneven and it may change in appearance over time.
Some other less common types of skin cancer include: Merkel Cell Carcinoma, Sebaceous Carcinoma, Dermatofibrosarcoma Protuberans (DFSP) and, Atypical Fibroxanthoma (AFX).
As with most types of cancer, early diagnosis and treatment of skin cancer leads to optimal outcomes.